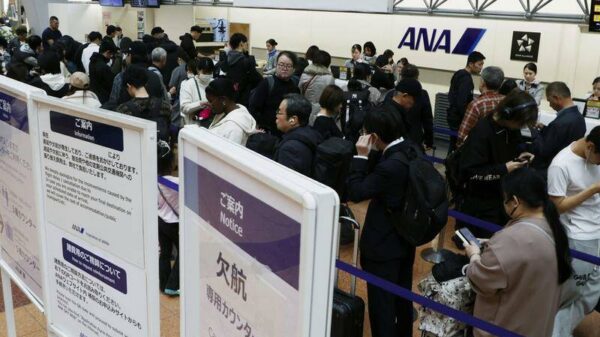
When uncontrolled wildfires spread from the foothills of Los Angeles into urban neighborhoods in January 2025, the immediate aftermath saw air quality deteriorate dramatically. Residents faced evacuations, yet local hospitals did not experience the expected surge in emergency visits. A recent study led by the University of Washington and Kaiser Permanente Southern California offers insights into the health impacts of these fires and how individuals turned to virtual health care services during the crisis.
The study, published on November 26 in JAMA Health Forum, analyzed health records from approximately 3.7 million Kaiser Permanente members. Researchers discovered a notable increase in health care visits, particularly for virtual consultations. Following the ignition of the fires on January 7, 2025, members reported a 42% rise in virtual visits related to respiratory symptoms. Those living near the burn zones experienced a 44% increase, while individuals throughout Los Angeles County logged 40% more virtual cardiovascular visits than anticipated.
The researchers estimated that during the first week of the fires, there were an excess of 27,903 respiratory outpatient visits, 18,489 respiratory virtual visits, and 15,792 cardiovascular virtual visits. This pattern suggests that during climate-related emergencies, people may increasingly depend on virtual health services, highlighting the need for healthcare providers to enhance their telehealth offerings in future crises.
Joan Casey, an associate professor of environmental and occupational health sciences and epidemiology at the University of Washington, led the research. “We saw over 6,241 excess cardiorespiratory virtual visits in the week following the fire ignition. This represents a substantial increase in care,” Casey stated. She emphasized that while the fires had a clear impact on health, the availability of virtual care allowed providers to effectively meet many patients’ needs during the ongoing disaster.
In collaboration with Kaiser Permanente Southern California, a health care system serving millions, the study defined exposure levels to the wildfires. High exposure indicated living within approximately 12 miles (20 kilometers) of a burn zone, while moderate exposure referred to residents of Los Angeles County situated more than 12 miles away. The researchers compared data from the weeks following the fires to a three-year baseline to predict healthcare visit patterns under typical conditions.
Besides the spikes in respiratory and cardiovascular visits, the study noted increases in consultations for injuries and neuropsychiatric symptoms. Outpatient injury visits among highly exposed individuals were 18% higher than expected, while virtual injury visits surged by 26% and 18% among highly and moderately exposed groups, respectively. Neuropsychiatric outpatient visits also saw significant increases of 31% and 28% in the same groups.
The proximity to the fire zones played a crucial role in the volume of health care visits. Among those needing respiratory-related care, minimally exposed members experienced a 31% increase in virtual visits, while moderately exposed individuals saw a 36% increase. Those in highly exposed areas accounted for a 42% rise.
Lauren Wilner, a doctoral student of epidemiology at the University of Washington and co-author of the study, noted that traditional emergency preparedness typically focuses on increasing hospital bed capacity and clinic staffing. “This work highlights the importance of considering virtual care capacity,” Wilner emphasized. “This may be particularly true for climate disasters like wildfires, where individuals are advised to stay indoors or must evacuate, prompting them to seek care online if possible.”
The research was conducted with support from the National Institute on Aging and the National Institute for Environmental Health Sciences. Other contributors included Yuqian Gu, Gina Lee, and Sara Tartof of Kaiser Permanente Southern California; Lara Schwarz of the University of California, Berkeley; Timothy Frankland of Kaiser Permanente Hawaii; Heather McBrien and Nina Flores of Columbia University; Chen Chen and Arnab Dey of the Scripps Institution of Oceanography at UC San Diego; and Tarik Benmarhnia of the Scripps Institution and the University of Rennes in France.
Overall, this study underscores the evolving landscape of health care delivery during environmental emergencies, suggesting that telehealth services will be increasingly vital as the frequency and intensity of climate-related disasters rise.