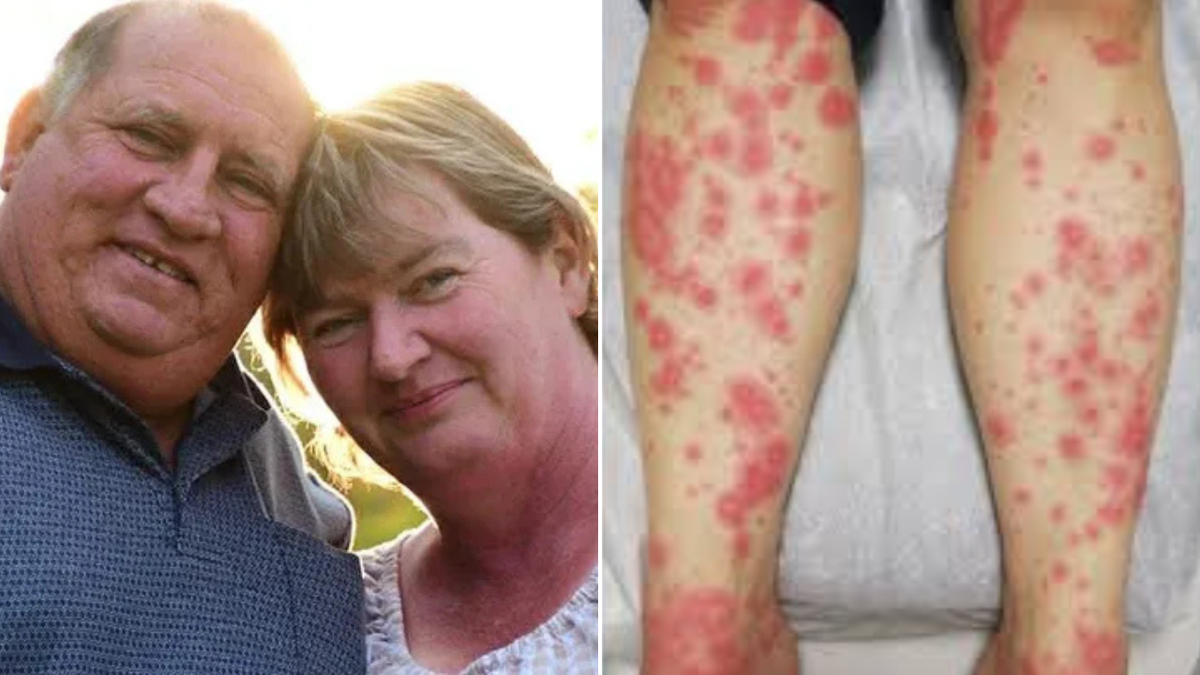
A mother of ten from New South Wales was airlifted to Sydney and admitted to intensive care after suffering a severe reaction to a routine antibiotic. Elizabeth Mohr, from Narrandera, experienced intense pain and a spreading rash starting on December 1, while she was being treated for a dental infection. Her condition deteriorated quickly over the following days, prompting urgent medical attention.
Samantha Mohr, Elizabeth’s daughter, reported that her mother visited Narrandera Hospital three times, each time leaving with prescriptions for antihistamines and steroids. Despite her worsening symptoms, including shivering and a lack of fever, medical staff deemed her case complex. Samantha described the situation in a GoFundMe page created to support the family, stating that by December 4, Elizabeth’s rash had become “aggressive” and she was not responding to treatments.
Ultimately, Elizabeth was transferred to Wagga Base Hospital, where doctors recognized the severity of her condition. She was airlifted overnight to Sydney, where specialists confirmed that the reaction was causing her body to overheat internally. Elizabeth received treatment as a burns patient in the intensive care unit for several days before being discharged just in time for Christmas. Samantha shared that the rash was essentially “burning her body from the inside out.”
According to Professor Deshan Sebaratnam, a dermatologist at The Skin Hospital, reactions to antibiotics can range from mild rashes to life-threatening conditions. He explained that while many patients experience minor side effects, some can develop severe reactions such as DRESS (Drug Reaction with Eosinophilia and Systemic Symptoms) or TEN (Toxic Epidermal Necrolysis). These conditions arise when the immune system reacts abnormally to medications, leading to inflammation in skin and internal organs.
Sebaratnam noted that distinguishing between mild and severe drug reactions can be challenging in the early stages, as symptoms often overlap. He criticized the current training in dermatology within Australian medical schools, claiming it is inadequate for preparing doctors to handle skin-related emergencies. “Many hospitals, even in major cities, do not employ dermatologists, making it difficult for patients to receive expert care,” he said. This issue is particularly pronounced in rural areas, where access to specialized medical professionals is limited.
The prevalence of severe drug reactions varies among different ethnic groups, with individuals of East Asian descent at a higher risk. Nevertheless, Professor Sebaratnam emphasized that anyone can experience these reactions. He stated that across Australia, only a few dozen cases of TEN occur each year, underscoring the rarity of such incidents.
Sebaratnam urged individuals to seek medical advice immediately if they develop a rash after beginning a new medication, particularly if symptoms worsen. He outlined several red flags to watch for, including painful rashes, facial swelling, formation of blisters or pus, involvement of the eyes, mouth, or genitals, and rashes that resemble bruises.
The case of Elizabeth Mohr serves as a critical reminder of the potential risks associated with antibiotic use and the importance of timely medical intervention when unusual symptoms arise.